Roll for Governor: A D&D Class Guide to California's Clown Car Election
Rolling those dice to determine how screwed we are.

Rolling those dice to determine how screwed we are.
Learn how to narrate an audiobook or make a zine, or dive into discussions around the politics of sideshow noise and the power of hauntings.
This week we have several queer proms, air quality, space balloons, miso, water fights, and more.
Naloxone, rescue breathing, and 911: Learn the do's, don'ts, and best practices for reversing an overdose.

In 2024, I responded to someone overdosing outside the newsroom where I worked. I’d carried naloxone on me for years, memorized exactly what to look for and what to do, and had seen many other people reverse overdoses in front me. However, I am not great in a medical emergency, and I was terrified I wasn’t going to be able to help this person stay with us.
Fortunately, the training I’d received from my harm reduction teachers over the years was burned into my brain. After a few scary minutes, I managed to help her start breathing again.
This is something anyone can do — a family member, a friend, or a stranger on the street — if they know what to look for.
Readers who don't use drugs, or aren’t intimately connected to people who do, might not ever be in this situation. However, being prepared gives us confidence to respond in a worst-case scenario, and to teach others these skills. Naloxone is a social intervention; while our public health systems are woefully inadequate, and the war on drugs continues unchecked, we can empower ourselves and one another to step up.
With that in mind, here’s how to respond to an overdose with compassion and care.
A note: The information below will teach you how to administer nasal naloxone, often called Narcan. Narcan is a brand of naloxone that controlled the market until its patent was broken a few years ago. It’s kind of like Kleenex, except if Kleenex charged $75 for life-saving medication during a health crisis where more than 100,000 people died of overdoses in a year. Your local pharmacy, like Walgreens (ironic) often has naloxone in stock.
Don’t ruin someone’s high for no reason! Make sure you know what to look for. A little science helps here: Opioids work by binding to receptors in the brain. This releases a large amount of dopamine, blocks pain, and slows down breathing. If someone is high, they can appear sleepy, and they may slump over. If their breathing is steady and regular, and they’re still responsive to someone saying their name loudly or shaking them, they’re not overdosing and don’t need naloxone.
Overdoses occur when someone’s body is overwhelmed by opioids and is so slowed down that they’re unresponsive and stop breathing. Their brain gets deprived of oxygen, and that’s when things get critical. Here’s how you can tell when that’s happening:
Signs of an overdose
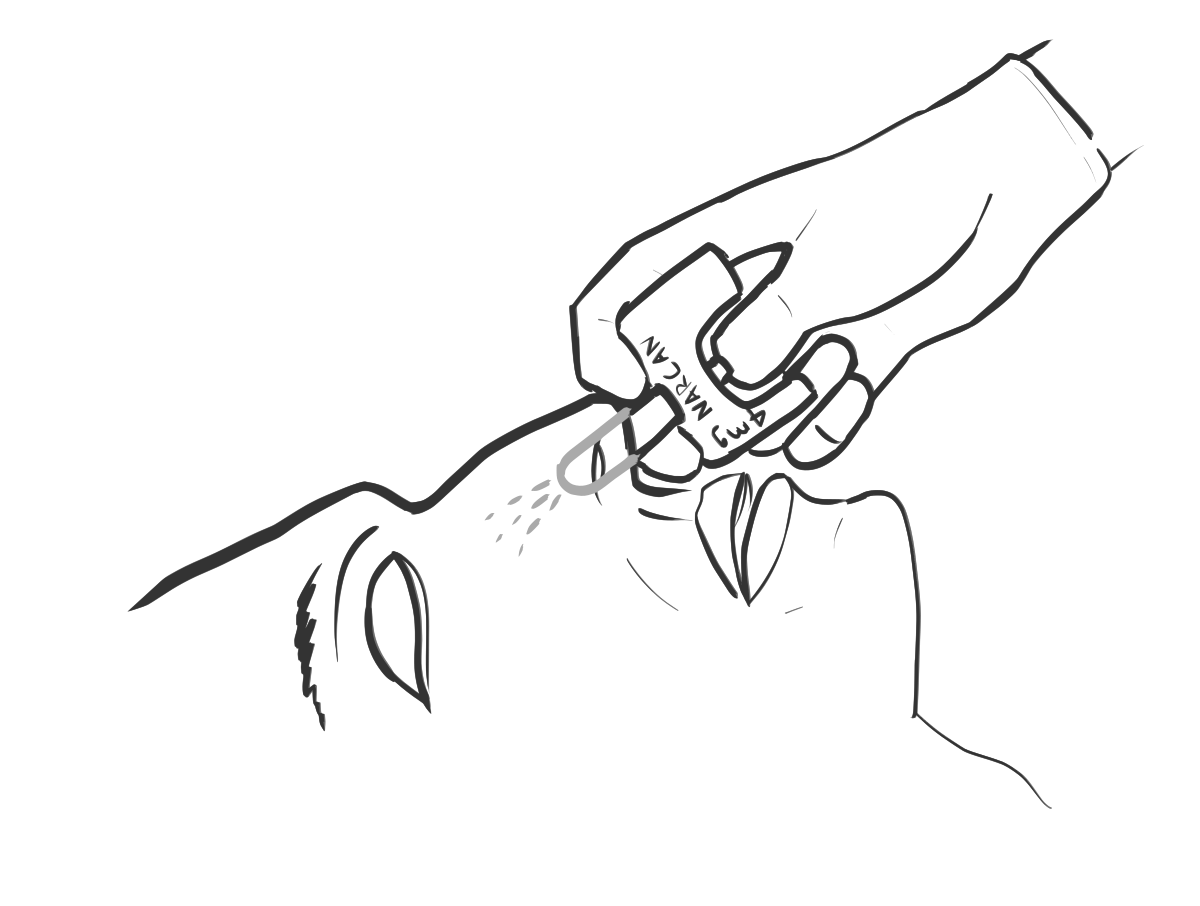
Should you call 911?
This is a tricky one. Calling the cops, especially in any scenario when drugs are involved and someone is in a vulnerable position, could invite more harm than good. However, if you don’t have naloxone, this is your first time responding to an overdose, someone isn’t coming round, and you’re worried there are other medical issues at play, calling in EMTs for backup is critical. You can do this right after you give them a dose. Cops won’t always tag along if it’s a health emergency. Saying “someone isn’t breathing” instead of “someone is overdosing” can help communicate to a dispatcher that there’s a health crisis at play that needs urgent response, and can circumvent prejudice toward people who use drugs.
Check in and see if they need anything, like food, water, help getting somewhere, or a call to a friend. Once you’ve gone your separate ways, take some time to process what happened. Responding to an overdose can be a stressful, adrenaline-fueled, emotional experience. Call a friend, have a good cry, curl up on the sofa and watch a silly movie. It may take you a little while to move through any feelings that come up, and that’s okay.

You have to inject a needle straight into their heart to reverse an overdose. Please do not do this. This is not Pulp Fiction.
People are angry and violent when they’re brought out of an overdose. Folks will have all sorts of responses, but they’re likely going to be confused, scared, nauseous, in a state of withdrawal, or have a pounding headache. Their state of being is okay! Don’t expect an outburst of gratitude. If you don’t feel safe, step away, and go find them a bottle of water.
The more naloxone you give someone, the better. If someone is not coming out of their overdose, and you’re waiting two minutes between each dose of naloxone, this could be true. But consider that the more naloxone someone receives, the farther it’ll send them into withdrawal, and the worse they’re going to feel when they’re conscious. Often it will take just one dose, maybe two. Health experts know this; that’s why RiVive, a new form of nasal naloxone on the market, has 3mg per dose, compared with the 4mg in Narcan. New high-dose versions, such as Kloxxado, which contains 8mg (!) of naloxone, is a favorite of law enforcement, which speaks for itself. It is not just unnecessary in most situations, but cruel and punishing toward people who would likely have been brought around with a lower dose.
People who use drugs don’t know how to take care of themselves. People who use drugs are experts in what they need. They care for one another, reverse each other’s overdoses, and their voices should be centered at every opportunity. Just because you know how to reverse an overdose doesn’t override their life experiences, or make you superior to them.
Learn more about naloxone and its many benefits at Remedy Alliance. For more information visit Next Distro and the National Harm Reduction Coalition. Safer Together offers local training in the Bay Area.

Nuala Bishari is an investigative journalist and opinion columnist who's reported on the Bay Area since 2013. She writes about public health, homelessness, LGBTQ+ issues, and nature.
View articles